The Human Lungs
Explore the anatomy and vital role of the lungs with Innerbody's interactive 3D model.
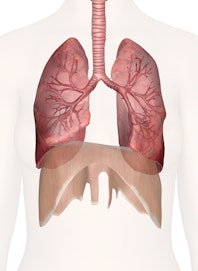
The human lungs are a pair of large, spongy organs optimized for gas exchange between our blood and the air. Our bodies require oxygen in order to survive. The lungs provide us with that vital oxygen while also removing carbon dioxide before it can reach hazardous levels.
If the inner surface of the lungs could be stretched out flat, they would occupy an area of around 80 to 100 square meters --- about the size of half of a tennis court! The lungs also provide us with the air we need in order to speak, laugh at jokes, and sing.
Anatomy of the Lungs
Pleura
The pleura are double-layered serous membranes that surround each lung. Attached to the wall of the thoracic cavity, the parietal pleura forms the outer layer of the membrane. The visceral pleura forms the inner layer of the membrane covering the outside surface of the lungs.
Between the parietal and visceral pleura is the pleural cavity, which creates a hollow space for the lungs to expand into during inhalation. Serous fluid secreted by the pleural membranes lubricates the inside of the pleural cavity to prevent irritation to the lungs during breathing.
External Anatomy
Occupying most of the space within the thoracic cavity, the lungs extend laterally from the heart to the ribs on both sides of the chest and continue posteriorly toward the spine. Each soft, spongy lung is roughly cone-shaped with the superior end of the lung forming the point of the cone and the inferior end forming the base. The superior end of the lungs narrows to a rounded tip known as the apex. The inferior end of the lungs, known as the base, rests on the dome-shaped diaphragm. The base of the lungs is concave to follow the contour of the diaphragm.
The left lung is slightly smaller than the right lung because 2/3 of the heart is located on the left side of the body. The left lung contains the cardiac notch, an indentation in the lung that surrounds the apex of the heart.
Each lung consists of several distinct lobes. The right lung (the larger of the two) has 3 lobes --- the superior, middle, and inferior lobes. The horizontal fissure separates the superior lobe from the middle lobe, while the right oblique fissure separates the middle and inferior lobes. The smaller left lung only has 2 lobes --- superior and inferior --- separated by the left oblique fissure.
Bronchi
Air enters the body through the nose or mouth and passes through the pharynx, larynx, and trachea. Just before reaching the lungs, the trachea then splits into the left and right bronchi --- large, hollow tubes made of hyaline cartilage and lined with ciliated pseudostratified epithelium. The hyaline cartilage of the bronchi forms incomplete rings shaped like the letter "C" with the open part of the ring facing toward the posterior end of the bronchi. The rigid hyaline cartilage prevents the bronchi from collapsing and blocking airflow to the lungs. Pseudostratified epithelium lines the inside of the hyaline ring and connects the unfinished ends of the ring to form a hollow tube shaped like the letter "D" with the flat part of the tube facing the posterior direction. Each lung receives air from a single, large primary bronchus.
As the primary bronchi enter the lungs, they branch off into smaller secondary bronchi that carry air to each lobe of the lung. Thus, the right bronchus branches off into 3 secondary bronchi while the left lung branches off into 2 secondary bronchi. The secondary bronchi further branch into many smaller tertiary bronchi within each lobe. The secondary and tertiary bronchi improve the efficiency of the lungs by distributing air evenly within each lobe of the lungs.
The pseudostratified epithelium that lines the bronchi contains many cilia and goblet cells. Cilia are small hair-like cellular projections that extend from the surface of the cells. Goblet cells are specialized epithelial cells that secrete mucus to coat the lining of the bronchi. Cilia move together to push mucus secreted by the goblet cells away from the lungs. Particles of dust and even pathogens like viruses, bacteria, and mold in the air entering the lungs stick to the mucus and are carried out of the respiratory tract. In this way mucus helps to keep the lungs clean and free of disease.
Bronchioles
Many small bronchioles branch off from the tertiary bronchi. Bronchioles differ from bronchi both in size (they are smaller) and in the composition of their walls. While bronchi have hyaline cartilage rings in their walls, bronchioles are made of elastin fibers and smooth muscle tissue. The tissue of the bronchiole walls allows the diameter of bronchioles to change to a significant degree. When the body requires greater volumes of air entering the lungs, such as during exercise, the bronchioles dilate to permit greater airflow. In response to dust or other environmental pollutants, the bronchioles can constrict to prevent the pollution of the lungs.
The bronchioles further branch off into many tiny terminal bronchioles. Terminal bronchioles are the smallest air tubes in the lungs and terminate at the alveoli of the lungs. Like bronchioles, the terminal bronchioles are elastic, capable of dilating or contracting to control airflow into the alveoli.
Alveoli
Alveoli are the functional units of the lungs that permit gas exchange between the air in the lungs and the blood in the capillaries of the lungs. Alveoli are found in small clusters called alveolar sacs at the end of the terminal bronchiole. Each alveolus is a hollow, cup-shaped cavity surrounded by many tiny capillaries.
The walls of the alveolus are lined with simple squamous epithelial cells known as alveolar cells. A thin layer of connective tissue underlies and supports the alveolar cells. Capillaries surround the connective tissue on the outer border of the alveolus. The respiratory membrane is formed where the walls of a capillary touch the walls of an alveolus. At the respiratory membrane, gas exchange occurs freely between the air and blood through the extremely thin walls of the alveolus and capillary.
Septal cells and macrophages are also found inside the alveoli. Septal cells produce alveolar fluid that coats the inner surface of the alveoli. Alveolar fluid is extremely important to lung function, as it is a surfactant that moistens the alveoli, helps maintain the elasticity of the lungs, and prevents the thin alveolar walls from collapsing. Macrophages in the alveoli keep the lungs clean and free of infections by capturing and phagocytizing pathogens and other foreign matter that enter the alveoli along with inhaled air.
Physiology of the Lungs
Pulmonary Ventilation
Our lungs receive air from the external environment through the process of negative pressure breathing. Negative pressure breathing requires a pressure differential between the air inside the alveoli and atmospheric air. Muscles surrounding the lungs, such as the diaphragm, intercostal muscles, and abdominal muscles, expand and contract to change the volume of the thoracic cavity. Muscles expand the thoracic cavity and decrease the pressure inside the alveoli to draw atmospheric air into the lungs. This process of drawing air into the lungs is known as inhalation or inspiration. Muscles can also contract the size of the thoracic cavity to increase the pressure inside of the alveoli and force air out of the lungs. This process of pushing air out of the lungs is known as exhalation or expiration.
Normal breathing involves several different mechanisms.
- Shallow breathing is accomplished by the contraction of the diaphragm and the external intercostal muscles for inhalation. During exhalation, the muscles relaxing and the elasticity of the lungs returning to their resting volume expels air out of the lungs.
- Our bodies accomplish deep breathing by a pronounced inferior movement of the diaphragm towards the abdomen. The external intercostal muscles along with the sternocleidomastoid and scalene muscles in the neck expand the space between the ribs, increasing the volume of the chest. During deep exhalation, the internal intercostal muscles and abdominal muscles contract to decrease the volume of the thoracic cavity, forcing air out of the lungs.
- Eupnea is the quiet breathing that happens when the body is at rest. During eupnea, the body mostly depends on shallow breathing with occasional deep breaths as the body needs slightly higher levels of gas exchange.
Lung Volume
The total air volume of the lungs is about 4 to 6 liters and varies with a person's size, age, gender, and respiratory health. Lung volumes are measured clinically by a device known as a spirometer. Normal shallow breathing only moves a small fraction of the lungs' total volume into and out of the body with each breath. This volume of air, known as tidal volume, usually measures only around 0.5 liters. Deep breathing can force more air into and out of the lungs than during shallow breathing. The volume of air exchanged during deep breathing is known as vital capacity and ranges between 3 to 5 liters, depending on the lung capacity of the individual. There is a residual volume of around 1 liter of air that remains in the lungs at all times, even during a deep exhalation. Fresh air entering the lungs with each breath mixes with the residual air in the lungs so that the residual air is slowly exchanged over time even at rest.
External Respiration
External respiration is the process of exchanging oxygen and carbon dioxide between the air inside the alveoli and the blood in the capillaries of the lungs. Air inside the alveoli contains a higher partial pressure of oxygen compared to the blood in the capillaries. Conversely, blood in the lungs' capillaries contains a higher partial pressure of carbon dioxide compared to the air in the alveoli. These partial pressures cause oxygen to diffuse out of the air and into the blood through the respiratory membrane. At the same time, carbon dioxide diffuses out of the blood and into the air through the respiratory membrane. The exchange of oxygen into the blood and carbon dioxide into the air allows the blood leaving the lungs to provide oxygen to the body's cells, while depositing carbon dioxide waste into the air.
Control of Breathing
Breathing is controlled by the brain and may be controlled both consciously and unconsciously.
- Unconscious control of breathing is maintained by the respiratory center of the brainstem. The respiratory center monitors the concentration of gases in the blood and adjusts the rate and depth of breathing as needed. During exercise or other exertion, the respiratory center automatically increases the breathing rate to provide constant levels of oxygen to the blood. During rest, the respiratory center reduces the breathing rate to prevent hyperventilation and maintain healthy oxygen and carbon dioxide levels in the blood.
- Conscious control of breathing is maintained by the cerebral cortex of the brain. The cerebral cortex may override the respiratory center and often does so during activities such as speaking, laughing, and singing. Unconscious control of breathing resumes as soon as conscious control of breathing ends, preventing the body from suffocating from lack of breathing.
Lung Disease
There are many diseases and conditions impairing the normal function of our lungs, even leading to death. You may be interested in learning more about how DNA health testing can screen you for genetic risk of an underdiagnosed hereditary condition called alpha-1 antitrypsin deficiency.










